Chinese Journal of Tissue Engineering Research ›› 2015, Vol. 19 ›› Issue (4): 634-641.doi: 10.3969/j.issn.2095-4344.2015.04.025
Previous Articles Next Articles
Comparison of anterior and posterior approaches for thoracolumbar burst fracture: a meta-analysis on Cobb angle loss, Frankel grading improvement and vertebral height loss
Aikeremujiang•Muheremu1, 2, 3, Sun Yu-qing1, Wu Zhong-yan3, Tian Wei1
- 1Beijing Jishuitan Hospital, Beijing 100035, China; 2Medical Center of Tsinghua University, Beijing 100084, China; 3The Fifth Affiliated Hospital of Xinjiang Medical University, Urumqi 838010, Xinjiang Uygur Autonomous Region, China
-
Revised:2014-11-14Online:2015-01-22Published:2015-01-22 -
Contact:Sun Yu-qing, Beijing Jishuitan Hospital, Beijing 100035, China -
About author:Aikeremujiang?Muheremu, Studying for doctorate, Physician, Beijing Jishuitan Hospital, Beijing 100035, China; Medical Center of Tsinghua University, Beijing 100084, China; The Fifth Affiliated Hospital of Xinjiang Medical University, Urumqi 838010, Xinjiang Uygur Autonomous Region, China
CLC Number:
Cite this article
Aikeremujiang•Muheremu, Sun Yu-qing, Wu Zhong-yan, Tian Wei. Comparison of anterior and posterior approaches for thoracolumbar burst fracture: a meta-analysis on Cobb angle loss, Frankel grading improvement and vertebral height loss[J]. Chinese Journal of Tissue Engineering Research, 2015, 19(4): 634-641.
share this article
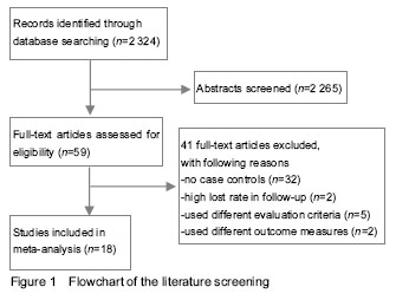
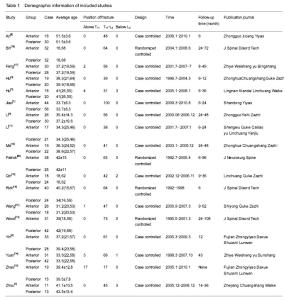
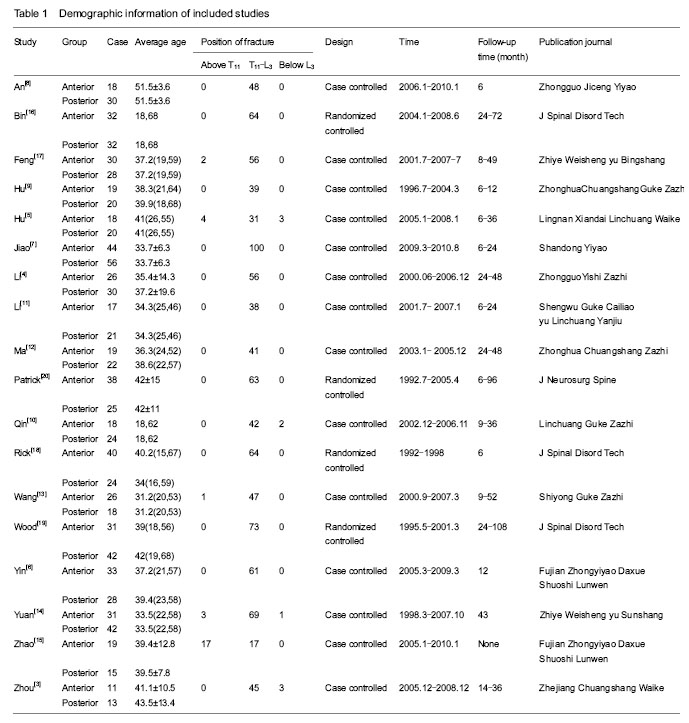
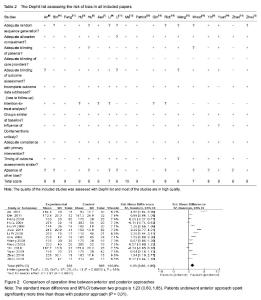
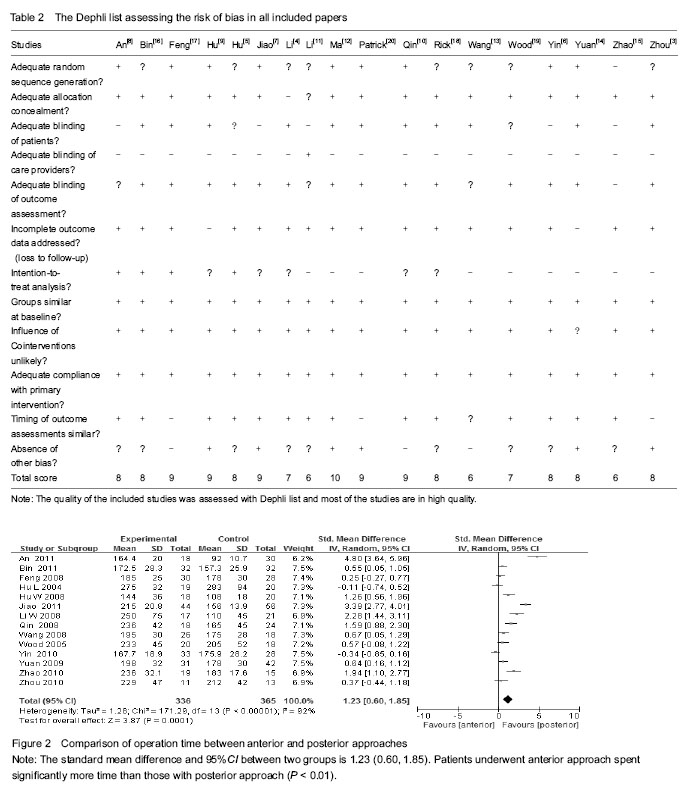
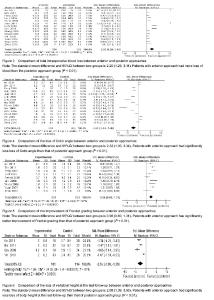
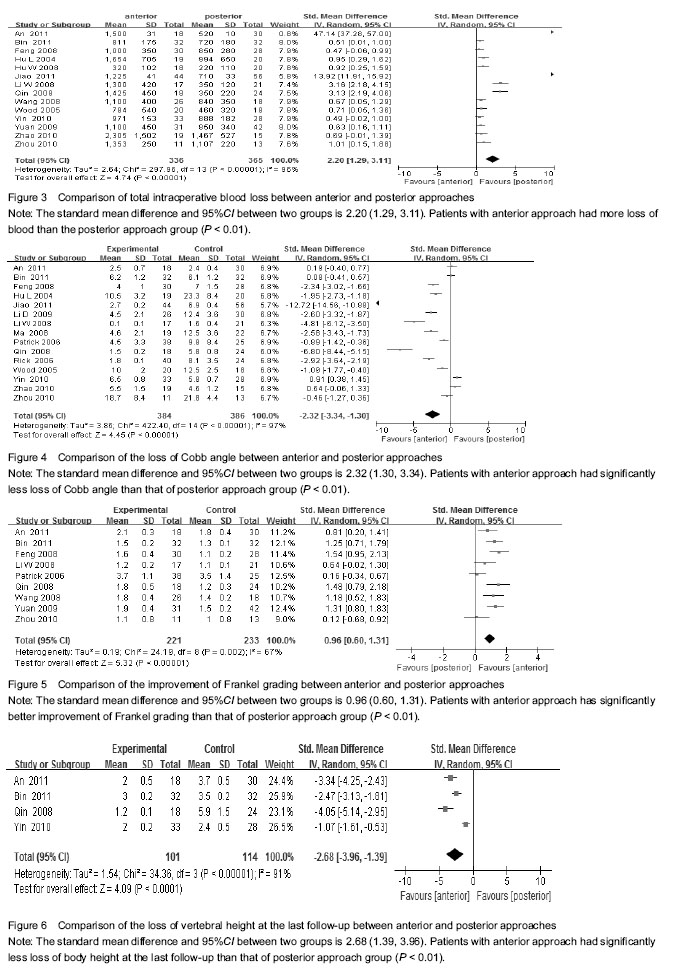
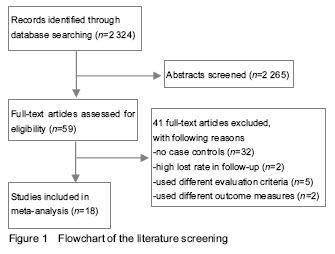
Results of literature retrieval Among the 2 324 papers screened, 18 papers were chosen for the final analysis[3-20] (Figure 1), including 4 English language papers and 14 Chinese language papers. The meta-analysis included a total number of 925 patients, 459 of whom were treated by anterior approach and 466 were treated with posterior approach (Table 1). Most studies were proved to be of relatively high quality assessing according the Dephli list of Cochrane Back Review Group[20] (Table 2). Meta-analysis on the operation time Fourteen studies[3, 5-11, 13-17, 19] including 736 patients (347 patients underwent anterior approach and 389 patients underwent posterior approach) have reported the time spent on the surgery. The standard mean difference and 95%CI between two groups is 1.23 (0.60, 1.85). Patients underwent anterior approach spent significantly more time than those with posterior approach (P < 0.01; Figure 2). Meta-analysis of the total intraoperative blood loss Fourteen studies[3, 5-11, 13-17, 19] including 707 patients (336 patients underwent anterior approach and 371 patients underwent posterior approach) have reported the total intraoperative hemorrhage. The standard mean difference and 95%CI between two groups is 2.2 (1.29, 3.11). Patients with anterior approach had more loss of blood than the posterior approach group (P < 0.01; Figure 3). Meta-analysis of the loss of Cobb angle at the last follow-up Fifteen studies[3-4, 6-12, 15-20] including 770 patients (384 patients applied anterior approach and 386 patients applied posterior approach) have reported the loss of Cobb angle at the last follow-up. The standard mean difference and 95%CI between two groups is 2.32 (1.30, 3.34). Patients with anterior approach had significantly less loss of Cobb angle than that of posterior approach group (P < 0.01; Figure 4). Meta-analysis of the improvement of Frankel grading Nine studies[3, 8, 10-11, 13-14, 16-17, 20] including 444 patients (221 patients applied anterior approach and 223 patients applied posterior approach) have reported the improvement of Frankel grading after the surgery. The standard mean difference and 95%CI between two groups is 0.96 (0.60, 1.31). Patients with anterior approach had significantly better improvement of Frankel grading than that of posterior approach group (P < 0.01; Figure 5). Meta-analysis of the loss of vertebral height at the last follow-up Four studies[6, 8, 10, 16] including 225 patients (101 patients applied anterior approach and 114 patients applied posterior approach) have reported the loss of spinal body height at the last follow-up. The standard mean difference and 95%CI between two groups is 2.68 (1.39, 3.96). Patients with anterior approach had significantly less loss of vertebral height at the last follow-up than that of posterior approach group (P < 0.01; Figure 6). In addition, three papers mentioned the changes in ASIA score after the surgery[2, 5, 15], all indicating that improvement of ASIA score after the surgery was significantly better in the anterior approach than the posterior approach; another study has reported significantly less loss of spinal canal volume at long-term follow visits in patients underwent anterior approach than those with posterior approach[5]. "
| [1] Muller U, Berlemann U, Sledge J, et al. Treatment of thoracolumbar burst fractures without neurologic deficit by indirect reduction and posterior instrumentation: bisegmental stabilization with monosegmental fusion. Eur Spine J.1999;8:284-289.
[2] Furlan AD, Pennick V, Bombardier C, et al. 2009 updated method guidelines for systematic reviews in the Cochrane Back Review Group. Spine (Phila Pa 1976). 2009;34(18): 1929-1941.
[3] Zhou JH, Ceng HB, Xu LF, et al. Comparative study of posterior 270° decompression and reconstruction via a posterior small incision approach and simple anterior decompression and fixation approach in treatment of severe thoracolumbar spine fracture. Zhejiang Chuangshang Waike. 2010;15(6):708-712.
[4] Li DY, Yang XJ, Zhou Z, et al. Comparison on the restoration of Cobb angle on patient with thoracolumbar burst fracture after anterior vs posterior surgical treatment. Zhongguo Yishi Zazhi. 2009;11(7):952-953.
[5] Hu WB, Huang WD, Su PQ. Surgical treatment of thoracolumbar vertebral burst fracture: anterior approach versus posterior approach. Lingnan Xiandai Linchuang Waike. 2008;8(4):267-273.
[6] Yin ZK. Comparative study about posterior and anterior approach for spine reconstruction with subtotal vertebretomy, decompreion and internal fixation for thoracolumbar vertebra burst fractures with spinal cord injuries. Fujian Zhongyiyao Daxue Shuoshi Lunwen, 2010.
[7] Jiao JB. Comparative study of anterior versus posterior surgical approach for the thoracolumbar burst fracture. Shandong Yiyao. 2011;51(20):93-94.
[8] An LY, Chen XH, Liu ZY, et al. Comparison on anterior versus posterior surgical approach for the thoracolumbar burst fracture. Zhongguo Jiceng Yiyao. 2011;18(16): 2227-2228.
[9] Hu L, Tian W, Liu B, et al. Selection of operation for old thoracolumbar fracture: anterior fixation versus posterior vertebral osteotomy. Zhonghua Chuangshang Guke Zazhi. 2004;6(11):1223-1225.
[10] Qin RJ, Li Y, Song B, et al. Comparison between anterior and posterior decompression and internal fixation in treatment of thoracolumbar burst fractures. Linchuang Guke Zazhi. 2008;11(2):115-118.
[11] Li WJ, Xie SW, Ma H, et al. Comparison between anterior and Posterior decompression and internal fixation in treatment of thoracolumbar burst fractures. Shengwu Guke Cailiao yu Linchuang Yanjiu. 2008;5(3):42-45.
[12] Ma H, Zhao J, Yu BQ, et al. Treatment of unstable thoracolumbar burst fractures: a comparison between anterior approach and posterior approach. Zhonghua Chuangshang Zazhi. 2008;24(8):602-604.
[13] Wang Z, Ouyang YC, Zhou Y, et al. Comparison between anterior and posterior surgical treatments of thoracolumbar burst fractures. Shiyong Guke Zazhi. 2008;14(11):641-643.
[14] Yuan XP, Zhang WJ, Liu W, et al. Comparison between anterior and posterior surgical treatments of thoracolumbar fractures. Zhiye Weisheng yu Sunshang. 2009;24(1):13-15.
[15] Zhao L. Comparative analysis on efficacy and posterior corpectomy for thoracic vertebral fractures. Fujian Zhongyiyao Daxue Shuoshi Lunwen, 2010.
[16] Lin B, Chen ZW, Guo ZM, et al. Anterior approach versus posterior approach with subtotal corpectomy, decompression, and reconstruction of spine in the treatment of thoracolumbar burst fractures a prospective randomized controlled study. J Spinal Disord Tech. 2011: 1-9.
[17] Feng J, Liang WJ, Li LF, et al. Comparison between anterior or posterior approach surgical treatment of thoracolumbar vertebra burst fractures. Zhiye Weisheng yu Bingshang. 2008;23(3):141-143.
[18] Rick CS, Ken R, Hanson D. Unstable thoracolumbar burst fracture: anterior-only versus short-segment posterior fixation. J Spinal Disord Tech. 2006;19(4):242-248.
[19] Wood KB, Bohn D, Mehbod A. Anterior versus posterior treatment of stable thoracolumbar burst Fractures without neurologic deficit: a prospective, randomized study. J Spinal Disord Tech. 2005;18(1):15-23.
[20] Patrick WH, James T, Eichholz K, et al. Comparison of anterolateral and posterior approaches in the management of thoracolumbar burst fractures. J Neurosurg Spine. 2006; 5: 117-125.
[21] Mahar A, Kim C, Wedemeyer M, et al. Short-segment fixation of lumbar burst fractures using pedicle fixation at the level of the fracture. Spine. 2007;32(14):1503-1507. |
| [1] | Chen Junming, Yue Chen, He Peilin, Zhang Juntao, Sun Moyuan, Liu Youwen. Hip arthroplasty versus proximal femoral nail antirotation for intertrochanteric fractures in older adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1452-1457. |
| [2] | Chen Jinping, Li Kui, Chen Qian, Guo Haoran, Zhang Yingbo, Wei Peng. Meta-analysis of the efficacy and safety of tranexamic acid in open spinal surgery [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1458-1464. |
| [3] | Hu Kai, Qiao Xiaohong, Zhang Yonghong, Wang Dong, Qin Sihe. Treatment of displaced intra-articular calcaneal fractures with cannulated screws and plates: a meta-analysis of 15 randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1465-1470. |
| [4] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Comparison of the short-term efficacy of extracorporeal shock wave therapy for middle-aged and elderly knee osteoarthritis: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(9): 1471-1476. |
| [5] | Wang Yongsheng, Wu Yang, Li Yanchun. Effect of acute high-intensity exercise on appetite hormones in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(8): 1305-1312. |
| [6] | Kong Desheng, He Jingjing, Feng Baofeng, Guo Ruiyun, Asiamah Ernest Amponsah, Lü Fei, Zhang Shuhan, Zhang Xiaolin, Ma Jun, Cui Huixian. Efficacy of mesenchymal stem cells in the spinal cord injury of large animal models: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(7): 1142-1148. |
| [7] | Song Chengjie, Chang Hengrui, Shi Mingxin, Meng Xianzhong. Research progress in biomechanical stability of lateral lumbar interbody fusion [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 923-928. |
| [8] | Huang Dengcheng, Wang Zhike, Cao Xuewei. Intravenous, topical tranexamic acid alone or their combination in total knee arthroplasty: a meta-analysis of randomized controlled trials [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 948-956. |
| [9] | Li Yan, Wang Pei, Deng Donghuan, Yan Wei, Li Lei, Jiang Hongjiang. Electroacupuncture for pain control after total knee arthroplasty: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 957-963. |
| [10] | He Xiangzhong, Chen Haiyun, Liu Jun, Lü Yang, Pan Jianke, Yang Wenbin, He Jingwen, Huang Junhan. Platelet-rich plasma combined with microfracture versus microfracture in the treatment of knee cartilage lesions: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 964-969. |
| [11] | Hua Haotian, Zhao Wenyu, Zhang Lei, Bai Wenbo, Wang Xinwei. Meta-analysis of clinical efficacy and safety of antibiotic artificial bone in the treatment of chronic osteomyelitis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 970-976. |
| [12] | Zhan Fangbiao, Cheng Jun, Zou Xinsen, Long Jie, Xie Lizhong, Deng Qianrong. Intraoperative intravenous application of tranexamic acid reduces perioperative bleeding in multilevel posterior spinal surgery: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(6): 977-984. |
| [13] | Zhong Yuanming, Wan Tong, Zhong Xifeng, Wu Zhuotan, He Bingkun, Wu Sixian. Meta-analysis of the efficacy and safety of percutaneous curved vertebroplasty and unilateral pedicle approach percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fracture [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 456-462. |
| [14] | Li Yang, Zhang Mingyong. Meta-analysis of the effect of double Endobutton and clavicular hook plate on the treatment of acromioclavicular dislocation [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 463-470. |
| [15] | Li Yanle, Yue Xiaohua, Wang Pei, Nie Weizhi, Zhang Junwei, Tan Yonghai, Jiang Hongjiang. Intramedullary nail fixation versus plate fixation in the treatment of displaced midshaft clavicular fractures in adults: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2021, 25(3): 471-476. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||